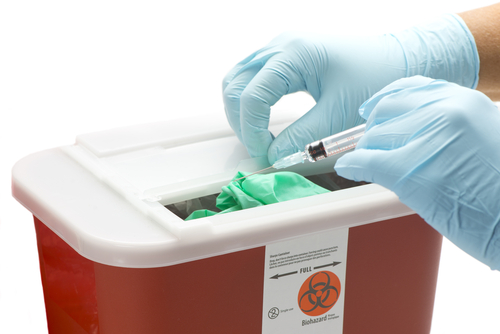
In this article, we will discuss the importance of properly disposing of biohazardous materials, such as sharps. Sharps contain infectious diseases and must be disposed of by a medical waste disposal company. In addition, this article will cover the different legal requirements related to the disposal of biohazardous materials. Also, we’ll explain why it’s important to use a licensed medical waste disposal company.
Sharps are a biohazardous material
The proper disposal of sharps requires following state regulations. Sharps contain blood-borne pathogens, which can infect people who are exposed to them. These pathogens can cause serious illness and even death. Some of the most serious diseases caused by bloodborne pathogens include AIDS and hepatitis. People who come into contact with these sharps often become very ill, and some of them even die.
To dispose of sharps properly, use an FDA-approved container. The container is made from puncture-resistant, rigid plastic and is labeled “Biohazard” or “Medical Waste.” Ensure that the sharps container is taped tightly and sealed before transportation. Place the container in a designated biohazard waste collection area. The container must be at least three-quarters full, and the lid should be tightly secured.
A sharps container is the proper way to store and dispose of biohazardous waste. These containers should be rigid and puncture-resistant. They must contain a biohazard symbol on them. The container should be closed tightly after use and should never be more than two-thirds full. In addition to using an approved container, sharps should be disposed of through your local medical waste contractor. The next section of this article will discuss proper disposal and handling.
In addition to sharps, other biohazardous waste materials should be separated. They should be properly identified, decontaminated, and disposed of. It is not safe to keep them in the public area for more than seven days. If possible, they should be removed by a designated person and transported to a biohazardous waste holding area. Pipettes, serological devices, and other items should be separate from other items.
They contain infectious disease
The Oregon Department of Environmental Health and Safety has rules for the safe disposal of sharps, which are medical waste that contain infectious disease. Sharps must be autoclaved, treated, or disposed of using methods approved by the Oregon Health Authority. After treatment, sharps may be disposed of at a landfill in a rigid container. The container must be clearly labeled and must be kept separate from other waste. Residents of Clackamas, Multnomah, and Washington counties may drop off their sharps at a transfer station. If the amount of sharps generated at a facility is less than 50 pounds per month, it is exempt from infectious waste disposal laws.
Disposing sharps can be a health hazard. These items can harbor infectious diseases and pose a threat to waste workers. Surgical instruments such as scalpels and needles are a common source of sharps. These items can accidentally enter recycling facilities or other places where humans may come in contact with them. Housekeepers and janitors are also at risk for injuries caused by loose sharps. In addition to these risks, the disposal of contaminated sharps may result in the transmission of diseases.
In addition to providing safe disposal options, hospitals should ensure that they maintain a safe environment by providing reusable sharps containers and educating patients. The containers must be leakproof and puncture-resistant, and employees must not attempt to clean or decontaminate sharps themselves. If sharps are not properly disposed of, staff members should monitor the location of their “kiosk” or “drop-off” containers.
They must be disposed of by a licensed medical waste disposal company
Whether you are a veterinarian, a dental office, or other medical professional, knowing the facts about sharps disposal is a must. Not only is proper sharps disposal important for the health of the public, but proper handling and disposal of these medical wastes can also protect the workers handling these wastes. Not only do discarded sharps expose waste workers to needle stick injuries and infection, but they can also be accidentally sent to recycling facilities, posing a serious risk to janitors and housekeepers. Even worse, used sharps can transmit serious diseases to people who have contact with them.
Most states require sharps disposal programs. If your state does not have any, you can place a sharps container in the middle of your trash bag. However, if you live in a state that does not offer sharps disposal services, you should take your container to a disposal facility. In Ohio, you can simply place the sharps container in the center of your regular trash bag. If you reside in other states, you should take your sharps container to a disposal center. You should not put it in the recycling bin and never return to a store to recycle sharps.
Remember that sharps should be stored in containers that are designed for disposing of sharp objects. Always use sharps disposal containers designed for this purpose and be sure to replace them every two-thirds full. It’s also helpful to keep sharps containers at eye level and within reach. If a reusable sharp is contaminated, it’s best to store it in a puncture-resistant container.
They are not regulated medical waste
The OSHA guidelines for the proper handling of hazardous waste include the rules for disposing of contaminated sharps. However, there are still a few requirements that differ from state to state. The OSHA Bloodborne Pathogen Standard specifies what constitutes a contaminated sharp. The term “contaminated sharp” includes anything that could contain a blood-borne pathogen, including scalpels, broken glass, capillary tubes, and exposed dental wire.
To dispose of sharps properly, they should be kept in a red, leak-proof container. The containers should be made of sturdy, puncture-resistant material and have strong seals to prevent leakage. Sharps containers should be sealed and properly labeled to warn of the biohazard content. Sharps waste containers should not be used for any other purpose besides disposal, and they must be tagged with the generator’s name.
It’s not enough to just dispose of sharps – proper management of these materials is essential for public health. In addition to posing a risk to waste workers and the public, improper management of these materials can result in infection and needle stick injuries. Furthermore, these sharps can be accidentally thrown away at recycling facilities, where they can endanger janitors and housekeepers. Sharps contain potentially harmful pathogens and are a major source of medical waste.
The State of New York oversees the Regulated Medical Waste Program, which provides guidelines and regulations for the safe disposal of regulated medical waste. Its mandated procedures include chemical disinfection, incineration, and thermal inactivation. Medical waste is generated by hospitals, residential health care facilities, diagnostic and treatment facilities, and clinical laboratories. However, the rules and regulations for their proper disposal differ from state to state.
They are subject to state and national regulations
Disposal of discarded sharps and other medical waste poses a health hazard to the public and waste workers. Inappropriate management of these materials can result in the transmission of dangerous diseases like HIV/AIDS. Additionally, improper disposal of sharps and other medical waste can contaminate the environment and the water supply. In developing countries, where sewage treatment is virtually nonexistent, poor management of discarded sharps and other medical waste can even lead to epidemics.
In non-hospital health care settings, the effects of NSPA are unclear. However, the 2012 Consensus Statement acknowledged the use of SIPFs in non-hospital settings. The study also addressed the need for more valid data on sharps injuries. The authors recommended that government agencies support research into the impact of NSPA in non-hospital settings and promote regional focus programs for enforcement of the BBP standard.
In the 1980s, concerns about the dangers of medical wastes were growing and the resulting beachfront cleanups resulted in Congress enacting the Medical Waste Tracking Act (MWTA). This two-year federal program was intended to reduce health risks associated with hazardous medical waste. The EPA promulgated medical waste management regulations on March 24, 1989. These regulations were then implemented in four states. They expired in 1991.
They are disposed of by autoclave or incineration
Autoclave or incineration is the preferred method for disposing of waste from medical procedures. Sharps are bulky and are difficult to treat with autoclave systems. The World Health Organization developed a costing tool to determine the amount of money and time required to treat the waste from surgery. Sharps are a small percentage of a hospital’s waste. The World Health Organization estimates that autoclave and incineration can save about $1 billion a year.
Incineration is the most popular method of disposing of sharps waste, but autoclave is not as common as incineration. It is important to follow the proper procedures to ensure the safety of medical waste disposal. Sharps waste should be collected in a proper container and stored separately until autoclaving is completed. After autoclaving, sharps waste should be disposed of incineration or discarded.
The disposal of biowaste cannot be thrown away in a regular trash bin. It must be collected in a red hard-wall biohazard waste collection container that can not exceed 15 gallons. This container must be lined with a clear autoclavable bag. NC State no longer accepts red/orange biohazard bag receptacles. To prevent the biohazard disposal of sharps, the container must be filled only 2/3 full.